Streptococcus pyogenes
A Microbiology Project by Charlotte Reese
Streptococcus pyogenes is not a bacteria that should be taken lightly. Many people carry the bacteria without
incident, however it has the potential to cause both mild and severe
diseases. Streptococcus
pyogenes has claimed many lives,
including that of Muppet's creator, Jim Henson. While most people will only suffer from mild infections,
such as strep throat or impetigo during childhood, it is important to
understand it's full pathogenic potential to understand how to identify, treat,
and avoid these infections.
Characteristically, Streptococcus pyogenes is a Gram-positive facultative anaerobic
bacterium. It is not motile, and
does not produce spores. It occurs
as long chains of cocci, and occasionally in pairs. Streptococcus pyogenes is classified as Group A streptococcus. Group A streptococci typically have a capsule composed of hyaluronic acid and are
beta-hemolytic, which is true for Streptococcus pyogenes.[1] Beta-hemolytic streptococci produce a toxin that forms a
clear zone of hemolysis on blood agar, demonstrating its ability to destroy red
blood cells. This hemolysis is
attributed to toxins formed by Group A streptococci called streptolysins. Streptolysins can destroy not only red
blood cells, but also the white blood cells responsible for fighting off
bacteria and disease, as well as other body cells.[2]
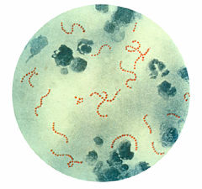
Figure 1
Streptococcus
pyogenes at 900x magnification
Several factors add to Streptococcus pyogene's
ability to cause disease.
These factors include its production of exotoxins and streptokinase, the
M proteins on its surface, and its hyaluronic acid capsule. Streptococcus pyogenes produces three types of exotoxins. These toxins are responsible for
causing fever and scarlet fever rashes; they also increase the risk of
endotoxic shock and depress antibody synthesis.[3] Streptococcus pyogenes also produces streptokinase, a toxin that digests blood
clots to assist in the invasion of wounds. The cell wall of Streptococcus pyogenes contains M proteins, which are a major factor behind its
virulence. M protein is heat and
acid resistant, it aids in the attachment to host tissues, and helps the cell
to resist phagocytosis. Host
immunity to Streptococcus pyogenes
results from the development of antibodies specific to M protein.[4] The hyaluronic acid capsule of Streptococcus
pyogenes is chemically similar to human
connective tissue, which allows it to go unrecognized as an antigen by the
host's body, further helping the bacteria to avoid phagocytosis.[5]
Streptococcus
pyogenes can be considered an opportunistic
pathogen. It is part of the normal
flora of the respiratory tract in many people, but usually does not cause
complications until the person's natural defenses to disease compromised.[5] Streptococcus pyogenes is somewhat unique in that it does not cause just one
disease, but is capable of causing many different diseases. These diseases range from mild, like
strep throat and impetigo, to severe, like necrotizing fasciitis,
and streptococcal toxic shock syndrome.
Streptococcus
pyogenes is the most common
bacterial cause of sore throat.[6] A painful, red throat with white patches on your tonsils is
characteristic of pharyngitis, otherwise known as strep throat. It is usually accompanied by swollen lymph
nodes, fever, and headache.
Occasionally it is also accompanied by nausea, vomiting, and abdominal
pain. Strep throat can be
diagnosed by a doctor through a throat culture or a rapid strep test.
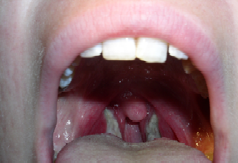
Figure 2
Reddened throat with white patches
on tonsils caused by
strep throat
If left untreated strep throat can lead to
further complications, including scarlet fever. Scarlet fever is characterized by a red rash on the chest
that may spread to the rest of the body.
The rash has a sandpaper-like texture and appears as tiny red pinpoints.[7] It is caused by the exotoxins produced
by Streptococcus pyogenes. Scarlet fever is
mainly seen in children under ten and can easily be diagnosed by a doctor by
the appearance of the rash.[8]
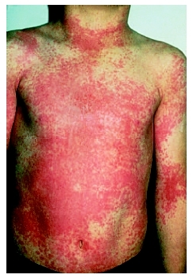
Figure 3
Characteristic rash of scarlet fever
Impetigo is another ailment caused by Streptococcus
pyogenes that is common among
children. Impetigo starts as a red
sore and form crusty sores after a few days. The sores most commonly occur on the face, but can also be
found on the extremities. They
usually itch, but are extremely contagious though direct contact, so scratching
the sores could spread the infection throughout the body.[7] A doctor can easily diagnose impetigo
through a visual examination of the sores.
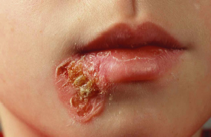
Figure 4
Crusty sore caused by
impetigo
Cellulitus
is an inflammation of the skin and deep tissues that can be caused by Streptococcus
pyogenes. Cellulitus begins when Streptococcus
pyogenes infects the site
of a minor injury, such as a bruise, burn, or wound. It causes the skin to turn red, widespread pain, swelling,
and tenderness of the infected area.
Other symptoms include fever and chills, swollen glands, blistering of
the skin, and malaise.[3]
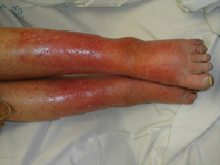
Figure 5
Redness and swelling
caused by cellulitus
Necrotizing
fasciitis is a rare, but very serious infection caused by Streptococcus
pyogenes that is
popularly termed "flesh eating bacteria". The bacteria typically enters the
body through a minor trauma or surgical wound in persons of compromised immune
systems and causes and infection just below the skin that spreads to deeper
tissues. Necrotizing fasciitis is
an extremely quick moving infection that is characterized by the rapid
destruction of tissue. It is fatal
in 30-40% of cases.[3]
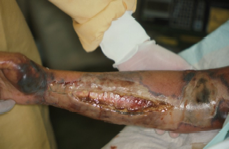
Figure 6
Extensive tissue
damage caused by nectrotizing fasciitis
Streptococcal
toxic shock syndrome is another very serious disease caused by Streptococcus
pyogenes. It is not the same as the toxic shock
syndrome associated with tampons, which can be attributed to Staphylococcus
aureus. Streptococcal
toxic shock commonly occurs in healthy individuals following an initial
infection of Streptococcus pyogenes. Symptoms include
significant pain, swelling, and redness of infected area, fever, dizziness,
difficulty breathing, dangerously low blood pressure, and a weak, rapid pulse.[9] Medical care is crucial as more than
50% of cases of streptococcal toxic shock develop into necrotizing fasciitis or
myositis, and there is a 30-70% mortality rate.[10]
Diseases
caused by Streptococcus pyogenes usually respond well to antibiotic treatment. The American Heart Association and the
Infectious Diseases Society of America currently recommend penicillin as the
drug of choice for treatment.[3] In severe cases, such as with necrotizing fasciitis,
surgical removal of the infected tissue may be required.
Streptococcus
pyogenes is most often
spread through contact with mucus or wounds of infected individuals. Due to this, thorough hand washing is a
good way to reduce the risk of becoming infected. The Center for Disease Control recommends that persons with
streptococcal infections stay home from work, school, or day care until they
have been taking antibiotics for at least 24 hours to reduce the risk of
transmitting the infection.[11]
References:
1.
Todar, Ken. 2005. "Streptococcus pyogenes and streptococcal Disease"
<http://www.bact.wisc.edu/themicrobialworld/strep.html>
2.
Tortora G, Funke B, Case
C. 2007. Microbiology: An Introduction, 9th Edition. Pearson Education, Inc.
3.
Sharma, Sat. 2006. "Streptococcus Group A Infections" <http://www.emedicine.com/med/topic2184.htm>
4.
Jevitz Patterson, Maria.
2004. "Streptococcus" <www.gsbs.utmb.edu/microbook/ch013.htm>
5.
Todar, Ken. 2002. "Streptococcus pyogenes" <http://textbookofbacteriology.net/streptococcus.html>
6.
Duckworth, Donna. 2006.
"Streptococcus pyogenes" <http://medinfo.ufl.edu/year2/mmid/bms5300/bugs/strpyoge.html>
7.
National Institute of
Allergy and Infectious Diseases. 2005. "Group A
Streptococcal Infections" <http://www.niaid.nih.gov/factsheets/strep.htm>
8.
Skin Care Guide Network.
2005. "Bacterial Infection Treatment - Strep pyogenes"
<http://www.skintherapyletter.com/treat/bacterial_infection/strep_pyogenes.html>
9.
Nemours Foundation.
2005. "Infections: Toxic Shock Syndrome" <http://www.kidshealth.org/parent/infections/bacterial_viral/toxic_shock.html>
10.Stevens,
Dennis. 1995. "Streptococcal Toxic-Shock Syndrome:
Spectrum of Disease, Pathogenesis, and New Concepts in Treatment" <http://www.cdc.gov/ncidod/EID/vol1no3/stevens.htm>
11.Center
for Disease Control, Division of Bacterial and Mycotic Diseases. 2005. "Group A Streptococcal (GAS) Disease" <http://www.cdc.gov/ncidod/dbmd/diseaseinfo/groupastreptococcal_g.htm>